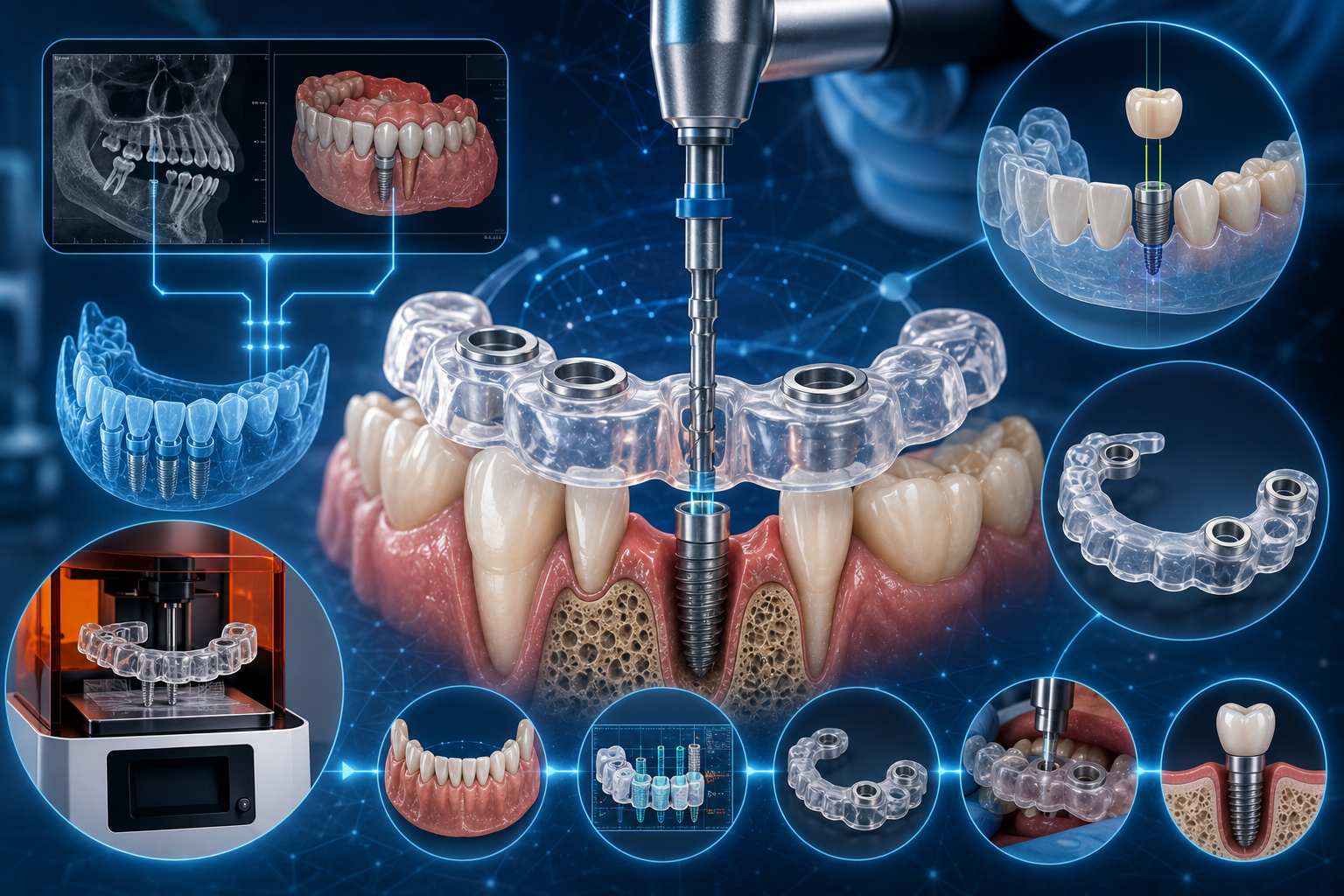
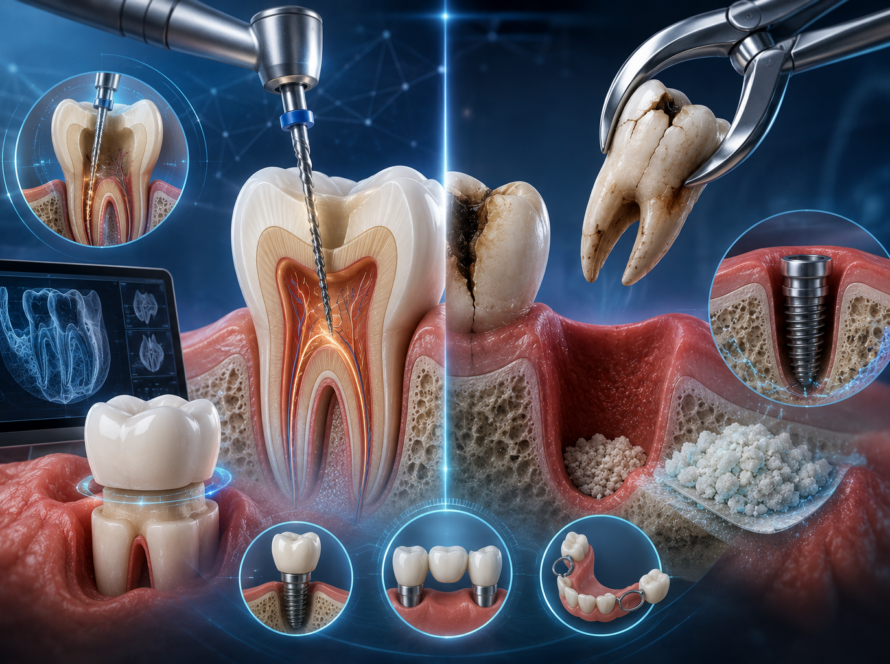
In the modern dental practice, “good enough” is no longer the standard for implantology. As we move through 2026, the shift from freehand surgery to 3D Guided Surgery has transitioned from a luxury to an essential clinical standard.
For the DenTrends community, staying at the forefront of DenTech means mastering not just the hardware, but the clinical protocols that ensure these tools deliver on their promise of micron-level accuracy. Here is the definitive clinical protocol for managing dental implant guides, from digital conception to surgical execution.
1. The Pre-Surgical Foundation: Data Merging
The success of a surgical guide is determined long before the patient sits in the chair. The “Double Scan” or “Data Merging” protocol is the bedrock of precision.
- Hard Tissue Data: High-resolution CBCT scans are mandatory to assess bone density, nerve pathways (IAN), and sinus positions.
- Soft Tissue Data: Intraoral scans (IOS) provide the “surface map” of the gingiva and dentition.
- The “Digital Handshake”: Use planning software (like coDiagnostiX or BlueSkyPlan) to merge the DICOM (CBCT) and STL (IOS) files.
Clinical Tip: Always verify the “fit” of the STL on the CBCT by checking the occlusal surfaces of remaining teeth. If the data alignment is off by even 0.5mm, the guide will fail.
2. Prosthetically-Driven Planning
We no longer place implants “where the bone is.” We place them where the tooth needs to be.
- Virtual Wax-up: Design the final crown first.
- Implant Positioning: Align the implant axis to emerge through the center of the virtual crown’s occlusal surface (for screw-retained) or cingulum (for anterior).
- Safety Zones: Maintain a minimum of 1.5mm from adjacent teeth and 3mm between implants to ensure biological width and vascularity.
3. Guide Design & Fabrication
Once the plan is locked, the guide is designed based on the support available:
- Tooth-Supported: The gold standard for stability in partially edentulous cases.
- Mucosa-Supported: Used for fully edentulous patients; often requires fixation pins to prevent “skating” during drilling.
- Bone-Supported: Primarily for complex cases involving significant bone reduction.
Manufacturing: 3D printing with biocompatible resins (e.g., Formlabs Dental SG) is now the industry standard, offering tolerances under 50 microns.
4. Intraoperative Management: The “Five-Check” Protocol
The most common point of failure is the clinical application of the guide. Follow this checklist:
- The Seating Check: Use “windows” or “ports” in the guide design to visually confirm that the guide is fully seated on the occlusal surfaces.
- Stability Test: There should be zero “rock” or movement. If using a mucosa-supported guide, engage the fixation pins before the first osteotomy.
- The Cooling Factor: Guided surgery restricts irrigation access. Use a pumping motion with the drill and ensure high-volume external cooling to prevent bone necrosis.
- Sleeve Calibration: Ensure you are using the correct “keys” or “spoons” for your specific guided kit. Misalignment here can lead to heat generation or stripping of the guide sleeve.
- Depth Control: Guided systems use physical stops. Trust the stop, but always verify the “offset” (the distance from the top of the sleeve to the implant platform) in your planning software.
5. Troubleshooting & Maintenance
Even with the best tech, clinical variables arise.
- Guide Fracture: If a guide cracks during surgery, immediately pivot to a backup traditional protocol or stop the procedure. Never “freehand” through a broken guide.
- Inadequate Opening: For posterior sites, if the patient has a limited opening, use “side-entry” guides or shortened drills designed for restricted space.
Final Thought
The data is clear: 3D surgical guides reduce surgical time by 30–40% and drop complication rates from approximately 10% to under 3%.
By following a strict digital-to-clinical protocol, you aren’t just placing an implant; you are executing a bio-engineered plan that ensures long-term prosthetic success and patient safety.