Speaker: DenTrends
Session Type: Basic Implantology
Foundations Every Dentist Must Know
This DenTalk session delivers a clear and structured introduction to dental implantology, focusing on biological principles, implant components, classifications, and clinical decision-making essential for predictable implant success.
What Is a Dental Implant?
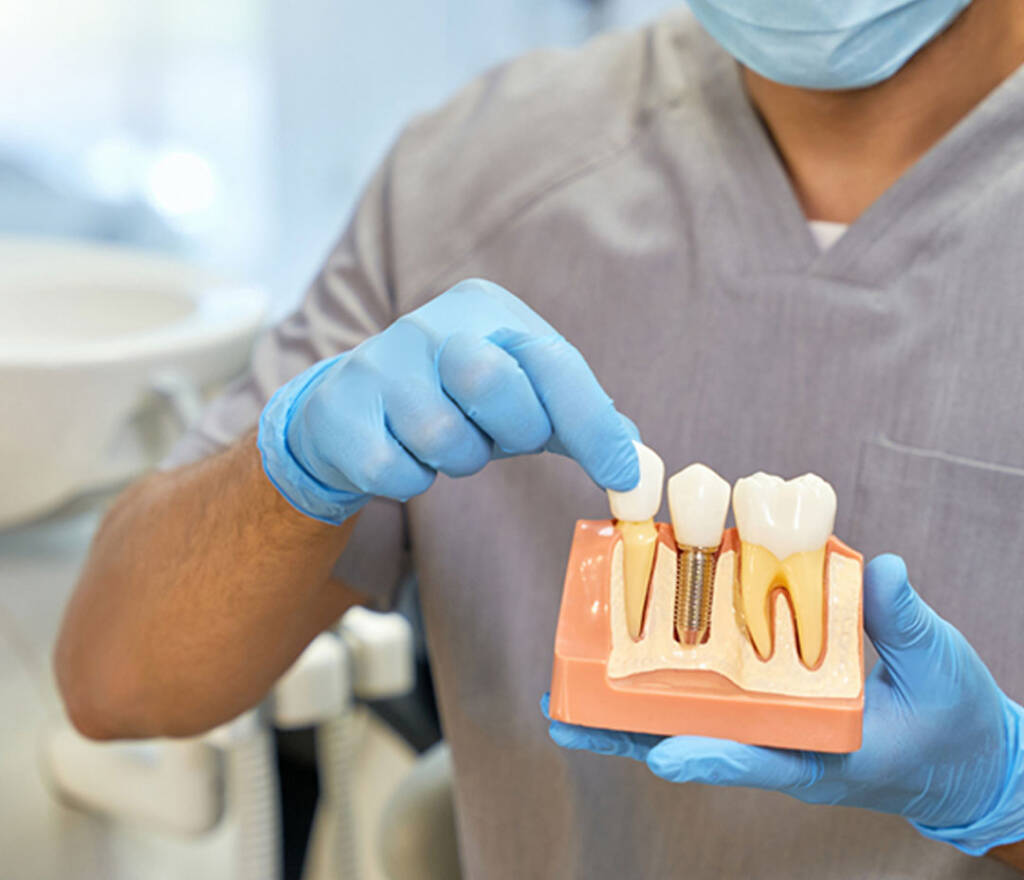
A dental implant is an artificial root surgically placed into the jawbone to support a prosthetic tooth or restoration. Typically designed as a screw-type fixture, the implant integrates with bone and later supports an abutment and prosthesis.
Components of a Dental Implant System
This session explains each component and its clinical role:
- Implant Fixture: Embedded within the bone
- Cover Screw: Seals the implant during initial healing
- Healing Abutment: Shapes peri-implant soft tissue
- Prosthetic Components: Transfer copings, impression copings, and analogs
Understanding components is critical for prosthetic accuracy and long-term stability.
Osseointegration: The Biological Key
Osseointegration is defined as a direct structural and functional connection between living bone and the implant surface.
Implant success depends on controlled bone healing and stable integration—without it, long-term function is impossible.
Classification of Dental Implants
Implants are classified based on:
- Anchorage: Endosteal, subperiosteal, transosseous, blade form
- Shape: Screw-type, blade-type
- Surface Texture:
- Pure titanium
- Acid-etched
- Porous-beaded
- Hydroxyapatite coated
Each modification aims to enhance bone contact and stability.
Natural Teeth vs Implants
Key differences highlighted in the session:
- Natural teeth have a periodontal ligament; implants do not
- Implants lack proprioception and adaptive movement
- Implants do not grow with bone → contraindicated in growing patients
- Occlusal overload and parafunctional habits increase failure risk
Indications for Dental Implants
Implants are indicated for:
- Replacement of missing teeth
- Improved mastication and speech
- Occlusal stability and space maintenance
- Orthodontic anchorage
- Preservation of alveolar bone
- Enhanced patient comfort and quality of life
Implant Materials and Longevity
- Commercial pure titanium remains the gold standard
- Titanium alloys and ceramic implants serve as alternatives
- Long-term success rates exceed 90% over 15 years, with many lasting decades under proper care
Risk Factors and Contraindications
Success can be compromised by:
- Uncontrolled systemic diseases (e.g., diabetes)
- Smoking, alcohol abuse
- Periodontal disease and bruxism
- Poor bone quality
- Poor oral hygiene and unrealistic patient expectations
Careful case selection is emphasized as non-negotiable.
Treatment Planning Essentials
A structured approach includes:
- Patient history and expectations
- Medical and dental risk assessment
- Clinical examination with periodontal charting
- Radiographic evaluation (OPG, CBCT)
- Clinical photography and study models
- Patient communication, consent, and cost transparency
Planning Aids and Surgical Accuracy
Key tools discussed:
- Diagnostic wax-ups
- Radiographic and surgical stents
- CBCT-based planning software
- Study casts, facebow records, and occlusal analysis
These tools ensure precise implant placement and prosthetic outcomes.
Impression Techniques for Implant Prosthetics
Two methods explained:
- Open Tray (Direct) Technique: High accuracy for multiple or angled implants
- Closed Tray (Indirect) Technique: Simpler cases with parallel implants
Correct impression transfer is essential for prosthetic fit and longevity.
Key Takeaways from This DenTalk
- Implant success depends on biology, planning, and precision
- Osseointegration is the cornerstone of implant therapy
- Proper component selection and impression technique are critical
- Patient selection and risk assessment determine long-term outcomes
- Implantology is predictable only when fundamentals are respected
DenTalk Conclusion
This DenTalk session provides a strong foundational framework for implant dentistry, preparing learners to advance confidently into surgical and prosthetic phases with biological awareness and clinical discipline.




