Speaker: DenTrends
Session Type: Dental Implants & Implant Surgery
Dental Implants & Implant Surgery
Dental implants are the gold standard for replacing missing teeth, offering function, stability, and long-term success when planned and executed correctly. This DenTalk session breaks down implant biology, components, surgical principles, and exam-relevant concepts in a concise, clinician-friendly format.
What Are Dental Implants?
The primary purpose of a dental implant is simple yet powerful:
to replace missing teeth by anchoring a prosthetic crown directly into bone.
Modern implants mimic natural tooth roots and integrate biologically through a process known as osseointegration.
Contraindications for Implant Placement
Not every patient is an ideal implant candidate.
Absolute / Relative Contraindications include:
- Uncontrolled diabetes
- Immunocompromised conditions
- Insufficient bone volume or height
- Bisphosphonate therapy (risk of BRONJ)
- Bruxism (heavy clenching/grinding)
- Smoking (relative)
- History of head & neck radiation
- Cleft palate patients
- Adolescents (implant placement delayed until jaw growth completion ~20–24 yrs)
Clinical Insight:
- Old age is NOT a contraindication
- Many implant contraindications overlap with extraction contraindications
Types of Dental Implants
Subperiosteal Implants
- Placed on top of bone, under periosteum
- No osseointegration
- Poor prognosis → obsolete
Transosseous (Transmandibular) Implants
- Pass completely through mandible
- Extraoral surgical approach
- Rarely used due to complexity
Endosteal Implants (Most Common)
- Placed into bone
- Root-form implants (cylindrical) are the modern standard
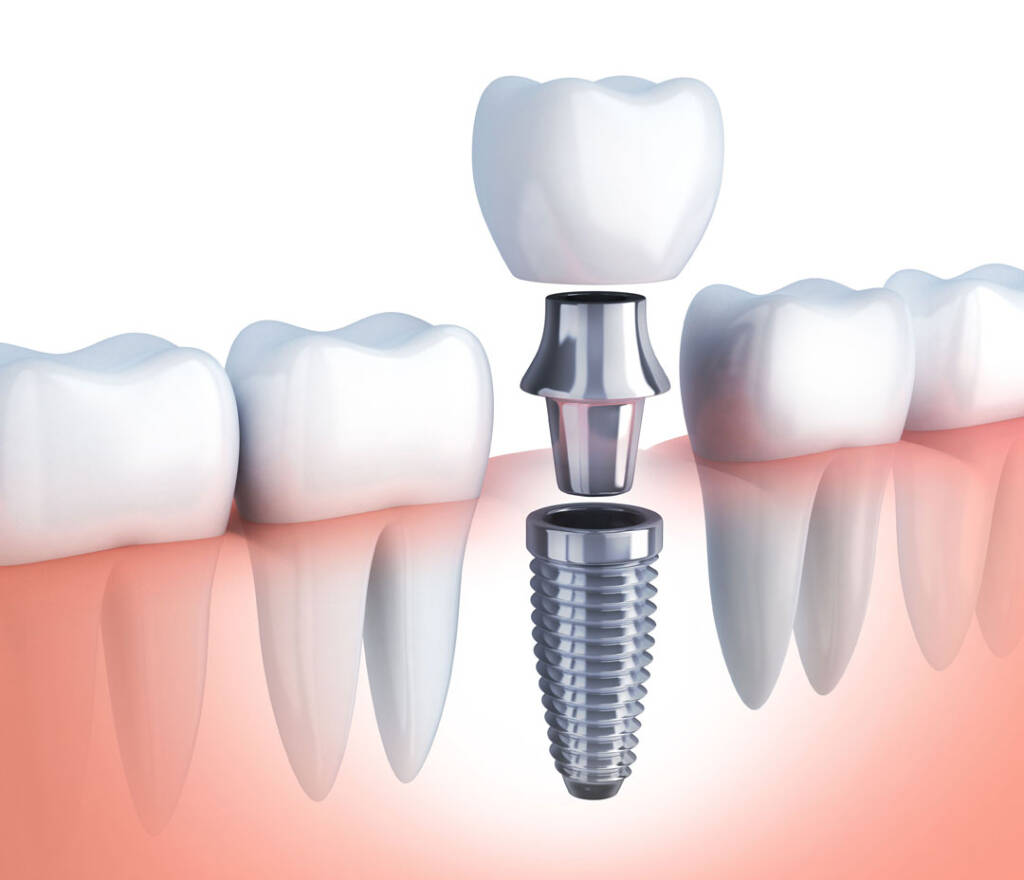
Components of an Endosteal Implant
From bottom to top:
- Implant body (fixture)
- Abutment
- Abutment screw
- Implant crown
Surgical Principles
- Sequential osteotomy
- Sharp drills + copious irrigation
- Prevents thermal damage and preserves bone vitality
One-Piece vs Two-Piece Systems
One-Piece Implants
- Implant + abutment fused
- No angulation correction
- Limited flexibility
Two-Piece Implants (Preferred)
- Implant body and abutment separate
- Allows angulation correction
- Better prosthetic control
Anti-Rotation Features
Prevent abutment movement:
- Internal hex
- External hex
Only present in two-piece systems
Implant Crowns
Screw-Retained Crowns
Pros:
- Retrievable
- No cement complications
- Requires less vertical space
Cons:
- Visible screw access
- Requires precise implant angulation
Cement-Retained Crowns
Pros:
- Superior esthetics (especially anterior)
Cons:
- Non-retrievable
- Risk of peri-implantitis from excess cement
Osseointegration & Stability
- Osseointegration: direct bone-implant contact → success
- Fibrous integration: mobility → failure
Stability Timeline
- Primary stability: mechanical (immediate)
- Dip phase: weeks 1–3
- Secondary stability: biological (bone healing)
Critical Safety Distances
- Adjacent tooth: ≥ 1.5 mm
- Inferior alveolar nerve: ≥ 2 mm
- Between implants: ≥ 3 mm
- Mental foramen: ≥ 5 mm
- Buccal / lingual bone: ≥ 1 mm
One-Stage vs Two-Stage Surgery
One-Stage
- Healing abutment exposed
- Single surgery
Two-Stage
- Implant buried under soft tissue
- Indicated for:
- Poor primary stability
- Bone grafting
- Medically compromised patients
Impression Techniques
- Open tray: most accurate
- Closed tray: simpler
- Impression coping + implant analog replicate implant position
Socket Preservation
After extraction:
- Atraumatic removal
- Bone graft placement
- Collagen membrane
- Primary closure not required
Soft Tissue & Biology
- Implants lack PDL
- Gingival fibers run parallel
- Rough surface → bone
- Smooth surface → soft tissue
Criteria for Implant Success
- ✔️ Immobile
- ✔️ No radiolucency
- ✔️ Minimal bone loss
- ✔️ No pain or infection
- ❌ Mobility
- ❌ Progressive bone loss
- ❌ Peri-implantitis
Thermal damage above 47°C compromises osseointegration
DenTalk Conclusion
Dental implant success is not accidental—it is the result of precise planning, biologic understanding, surgical discipline, and prosthetic accuracy. From bone quality to implant design, every decision impacts longevity. Mastering these fundamentals is essential for both clinical excellence and long-term patient outcomes.




